INTRODUCTION
Cervical spondylomyelopathy (CSM) is the most common cause of dysfunction of the spinal cord, affecting over 85% of patients over 60 years of age in the United States.1–5 CSM results from degenerative changes to the spinal joints and surrounding soft tissues, including the discovertebral joints, facet articulations, and ligamentum flavum, and can present with a broad range of symptoms from mild local pain to complete paralysis.1–3 Cervical disc extrusion, a severe form of disc herniation in which nuclear material breaches the annulus and extends beyond the disc space, represents a significant contributor to cervical radiculopathy and myelopathy in this population.
Non-surgical spinal decompression (NSD) has recently emerged as a promising conservative treatment option for lumbar disc herniation.6 In this study, we describe a case of a patient presenting with cervical pain, disc extrusion with cephalic migration, and segmental instability, and report the effect of a tailored multimodal treatment approach with NSD combined with other conservative therapies. Plain film radiography and MRI were utilized to evaluate changes in the C5/C6 intervertebral disc. The type of herniation was identified7 and herniation index was calculated as described previously.6
CASE REPORT
Patient Presentation and Outcome
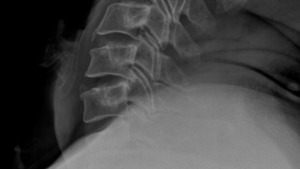
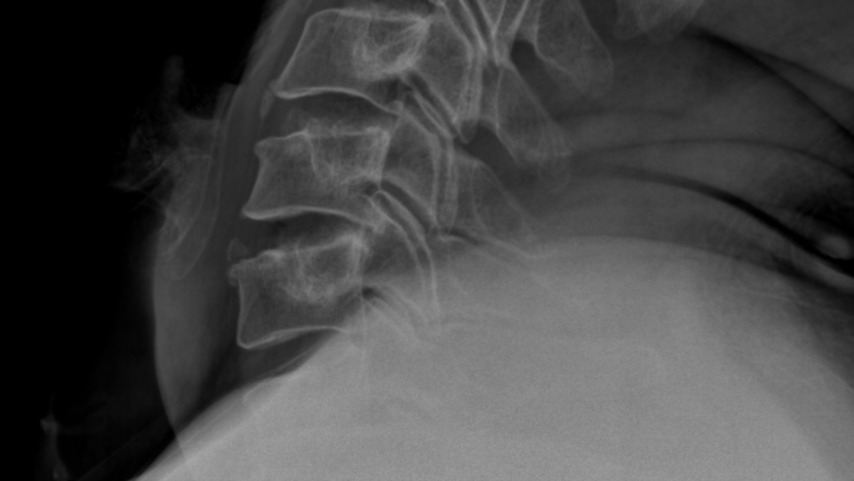
A 50-year-old male had slight neck pain, radiating to the left shoulder blade, numbness in left distal 2nd digit and slight tremors of the left 5th digit. The intensity of these symptoms ranged from a 4–8/10 on the Visual Analog Scale (VAS) and were occurring multiple times per day. All the patient’s symptoms were progressive during the past 4 months. No history of recent injury or acute pain in the last four months prior to presentation at the clinic. His chief complaint was waking up multiple times during the night with severe pain which was also present during walking, sitting, and other physical activities. Two months prior to attending the clinic, an MRI showed a C5/C6 disc extrusion. The herniation index of 382 was calculated based on MRI findings. During his initial visit, 4 cervical x-rays were obtained: AP, Lateral, Flexion and Extension. The x-rays revealed a retrolisthesis at C5 relative to C6 measuring 5.3 mm/18% translation (Figure 1). This indicated segmental instability at the C5-C6 level on extension. A diagnosis of cervical segmental instability with severe disc herniation was made. Anterior spinal fusion was recommended as the best course of treatment for the patient. However, the patient was seeking alternative options to invasive surgery.
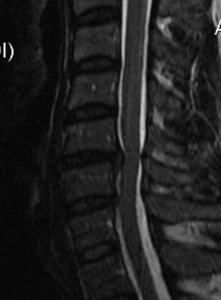
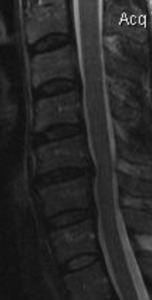
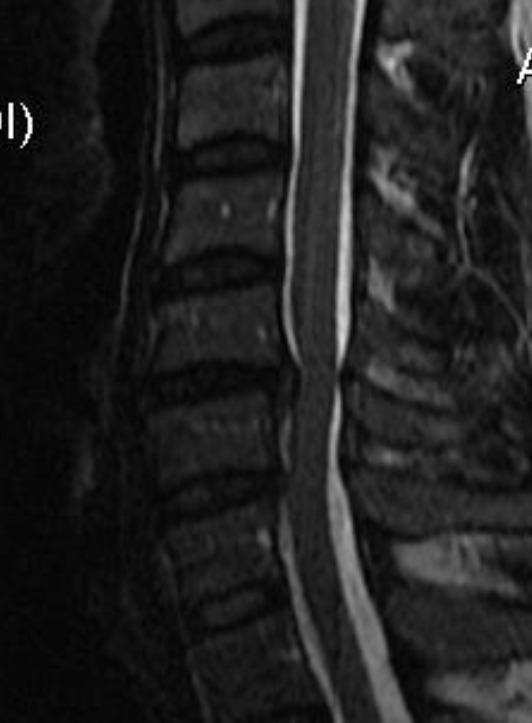
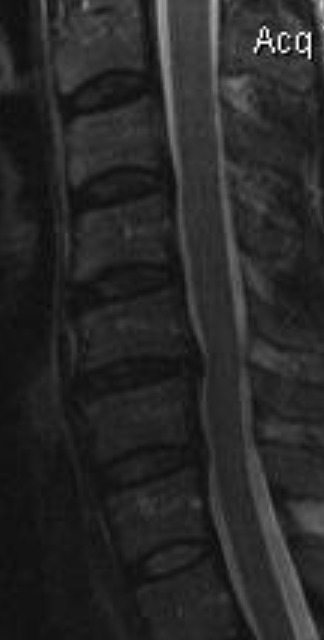
The treatment plan for this patient included a combination of NSD therapy with low-level light therapy, electrical muscle stimulation, strength training with power plate, cold pack, manual therapy and chiropractic adjustments for 3 months. Following this period, the patient reported 60% improvement in neck pain, shoulder blade pain, numbness and tremors with considerably reduced intensity and frequency. At 4 months the MRI showed reduced disc extrusion, with a herniation index of 283 or 26% reduction. The follow-up MRI a year later showed a 52% reduction of the C5/C6 disc extrusion with no increase in instability (Figures 2 and 3).
Imaging Analysis
Plain film studies were obtained on 3 different occasions (initial, 2 months and 5 months). The flexion and extension views revealed a persistent retrolisthesis of C5 relative to C6 on extension. This results in a dynamic stenosis of the spinal canal between the posterior inferior body margin of C5 and spinous lamina junction of C6. This is due to the pincer activity that potentially could occur during extension-related activities, contacting and narrowing the spinal cord. Additionally, there was a persistent increased angulation of the C5/C6 intervertebral disc on extension, representing an angle that is greater than 11° in difference relative to the adjacent segmental levels of C4/C5 and C6/C7 (Table 1). Segmental instability was indicated.
Assessment of Imaging Studies
Torg ratio. This was calculated as a sagittal diameter of the cervical canal divided by the sagittal diameter of the vertebral body on lateral radiographs and on mid-sagittal MRI (C5 level).8
Cervical lordosis. This measurement utilizes the tangential method of measurement or the C2/C7 angle to form an angle from the C2 through C7 vertebral level.8,9
Translation on plain film radiographs from flexion to extension: Translation of a vertebral body represents the movement of one segment relative to the segment below during flexion and/or extension activity. A forward displacement or translation of the segment relative to the vertebra below is referred to as anterolisthesis. A backward displacement of the segment above relative to the segment below is referred to as retrolisthesis. When a single segment develops a forward or backward movement relative to the segment below, instability is likely. In the literature, criteria for diagnosis of segmental instability is often defined by the White-Panjabi method10–12 as a displacement of greater than 3.5 mm/20% translation.10,11 However, this criteria was developed prior to MRI availability. The advantage of MRI is that soft tissue changes of the spinal canal can be evaluated to obtain a more specific definition for instability.13 We used flexion and extension studies of the cervical spine to identify intersegmental translational motion and MRI to detect soft tissue changes. The translation of the cervical segment together with changes in soft tissue visible on MRI studies provides an accurate definition of instability including stenosis.
Increased disc angulation: Disc angulation and translational motion are factors related to segmental instability. A disc angulation that is greater than 11° difference in relation to the angulation of adjacent vertebral segments indicates instability.10,11
Herniation index: The herniation index provides a method to compare an axial image of a disc herniation from one study to that of the patient in another study. The axial image creating the greatest distortion in disc herniation contour was utilized. The anteroposterior (AP) and width of the disc herniation was compared to the size of the spinal canal.6
Disc terminology: The published disc terminology of “bulge, protrusion, extrusion and sequestered disc” is most applicable to the lumbar spine. In considering a disc herniation of the cervical spine, the spinal cord takes up a considerable amount of space in the spinal canal, meaning that a smaller magnitude of disc bulge/herniation can produce symptomatic change. In addition, congenital stenosis of the canal is much more significant than in the lumbar spine.
Dynamic stenosis: The degree of stenosis changes with movement. This is referred to as the “pincer effect” and is a feature of segmental instability of the cervical spine. The sagittal canal diameter is measured and compared on flexion and extension films. Typically, this is corrected by surgical fusion.
Imaging Analysis
Plain film studies were obtained on 3 different occasions (initial, 2 months and 5 months). The flexion and extension views revealed a persistent retrolisthesis of C5 relative to C6 on extension. This results in a dynamic stenosis of the spinal canal between the posterior inferior body margin of C5 and spinous lamina junction of C6. This is due to the pincer activity that potentially could occur during extension-related activities, contacting and narrowing the spinal cord. Additionally, there was a persistent increased angulation of the C5/C6 intervertebral disc on extension, representing an angle that is greater than 11° in difference relative to the adjacent segmental levels of C4/C5 and C6/C7 (Table 1). Segmental instability was indicated.
MRI studies were performed on three different occasions during the period of evaluation of this patient. The MRI studies demonstrated a reduction in the herniation index (approximately 50%) from the initial presentation to the final evaluation of the patient at the intervertebral disc (Table 2).
The cephalocaudal vertical measurement is the measurement of the disc extrusion from top to bottom as visualized on sagittal images.
Treatment Protocol
The patient received 30+ NSD treatments at 2-3 times per week over a 3-month period. The details of NSD treatment protocol are described in our previous publication.6
DISCUSSION
CSM represents the clinical result of a degenerative process of the spinal joints and surrounding soft tissues in the neck, including the discovertebral joints, facet articulations, and ligamentum flavum.1–3 Spinal degeneration generally takes decades to develop and is therefore most prevalent in the elderly population and is slightly more common in males.4 The natural course of the disease is not continuously progressive and often presents with latency periods followed by rapid neurological decline.1,3 The diagnosis of CSM is based on an accumulation of findings including clinical presentation as well as physical and imaging exam findings.1 The most universally used metric for grading is the Japanese Orthopedic Association (JOA) Scale, with scores of 13–17 considered mild, 10–12 moderate, and 0–9 severe.1,14 CSM can be assessed on a variety of imaging modalities, including conventional radiography, computed tomography, or the gold standard, magnetic resonance imaging.1–3 The Torg-Pavlov ratio is often employed when assessing for central canal stenosis; ratios <0.8 indicate stenosis.1,3
Surgical decompression is universally accepted as the treatment of choice for moderate to severe CSM. However, controversy arises over the management of mild presentations.1,2,14–17 Many reports reveal satisfactory results following conservative cervical traction management with a tolerance of 70%, and others show an improvement with conservative traction in 50% of patients.1,14,18 When comparing JOA scores of pre and post conservative management, one study found at least half the participants improved by at least one grade and a level of “no disability” was achieved in around 25%.16 Opponents to conservative management argue that 20% of patients under conservative management regress neurologically and eventually undergo surgical decompression.1 When comparing the long-term effects of patients who underwent surgical versus conservative management, some researchers found no statistical difference in patient outcomes.17,19,20 Complications of surgical approaches include dysphagia, nerve palsies, pseudoarthroses, vascular injuries, Horner’s syndrome, and hardware failures, with complication rates of 15.6% within 30 days of surgery and 4.4% from 30 days to 2 years.3
In the last 3 decades neck pain has remained as a highly prevalent disability world-wide,21 despite availability of a broad spectrum of treatment modalities ranging from conservative therapies,22–26 to pharmacotherapies22 and surgical interventions27,28 with limited long-term effectiveness. In parallel to the significant impact of LBP on economics and healthcare systems,29,30 neck pain has been one of the leading contributors to global disability21 ranking second to LBP for years lived with disability among musculoskeletal conditions.31 Considering that chronic neck pain can be associated with progressive disc degeneration and segmental cervical instability causing severe pain and dysfunction,32 timely treatment is critical to prevent further progression of this debilitating condition. In the current case study, we report a patient with symptomatic cervical disc herniation and diagnosed instability. We demonstrated significant reduction in pain intensity, improved function, sensory abnormalities and quality of life in this patient by combining NSD with other chiropractic modalities. These improvements and resolution of symptoms were maintained at one year follow-up.
The primary source of chronic neck pain is thought to involve destabilisation of the cervical spine as a result of capsular ligament laxity and dysfunction of the cervical facet joints.33 Other underlying mechanisms of spinal instability have been proposed to involve changes in deep cervical flexors and extensor muscle composition leading to impaired physical function and pain.34 As a consequence of underlying cervical instability, radicular pain and degeneration of the cervical discs can occur resulting in cervical radiculopathy which is associated with spondylosis.33 Diagnosis is based on clinical examination and confirmed by functional radiological investigations that facilitate assessment of cervical instability pathology.8,35 The non-invasive NSD therapy utilizes a controlled computerized feedback mechanism36 to deliver repetitive forces to accurately target the herniated disc by considerably reducing intravertebral disc pressure (from -100 to -600 mmHg).37 This negative pressure on nerve roots reduces stress on facet joints,37,38 leading to improved uptake of nutrients and oxygen, expansion of intervertebral space and facilitation of disc height restoration, thus alleviating compression-associated symptoms.39,40
Although there are limited clinical studies published on the efficacy of NSD for treatment of segmental cervical instability, the consistent findings of statistically significant improvements in cervical symptoms associated with intervertebral disc herniation and cervical radiculopathy indicate promising utilization of NSD as part of a multimodal rehabilitation treatment approach.36,37,39–44 A randomized controlled trial of patients with multisegmented cervical disc herniation demonstrated significant resolution of symptoms of cervical intervertebral disc degeneration and improved muscle relaxation compared to conventional traction.43 Similarly, a more recent randomized controlled trial on the impact of spinal decompression therapy in patients with cervical herniation found that both disability and pain scores were significantly reduced in the experimental group (NSD plus conventional physiotherapy) compared to the control group (conventional physiotherapy alone).41 A number of cohort studies36,45–47 and recent case reports42,44 have also shown considerable improvement in pain levels and functional activity in patients with chronic neck and herniated or degenerative disc following treatment with NSD combined with other conservative therapies. Collectively, the findings of this clinical case and previous trials support the benefit of NSD as adjunctive to other rehabilitation therapies in management of cervical spine disorders.
The findings of our study also highlight the diagnostic importance of imaging findings to identify degenerative or herniated cervical discs and monitor the progress of clinical improvement in pain and function of such patients. The imaging findings of a retrospective study of patients with CSM and mild to moderate cervical spinal cord compression indicated that cervical segmental instability, a high intramedullary signal detected on MRI and reduced Torg ratio correlated strongly with myelopathy signs and symptoms.8 In addition, a more recent retrospective study highlighted the diagnostic value of cervical spine radiographs to assess cervical spine instability and canal stenosis with further evaluation of spinal cord pathology using MRI in young men (<30 years) diagnosed with non-herniated degenerative CSM.35 Congenital cervical stenosis and mild sagittal malalignment of the cervical spine were identified on radiographs, with MRI confirming the presence of degenerative discs, spinal cord compression and intramedullary abnormal intensity lesions. The resulting segmental instability, exacerbated by congenital canal stenosis, further accelerated spinal cord compression and damage.35
The current case study on the use of NSD for clinical management of cervical spine instability associated with chronic neck pain provides additional evidence to support the mainstream application of a non-invasive multimodal approach. Based on limited controlled trials investigating clinical effectiveness of NSD for cervical symptoms, therapeutic efficacy remains to be confirmed. However, statistically significant improvements from cohort studies and case reports provide grounds for further exploration.
CONCLUSION
This study supports the use of NSD therapy in the management of chronic neck pain and cervical instability. The considerable decrease in pain and disability as well as the absence of adverse effects in our patient indicate the potential efficacy and safety of the procedure. We also highlight the importance of MRI and cervical x-rays in facilitating accurate diagnosis of cervical instability and monitoring of outcomes. Future controlled trials are warranted to advance clinical and translational research of NSD for treatment of cervical instability.