INTRODUCTION
This paper describes a second case of an incidental teratoma in a patient in a chiropractic clinic.1 Teratomas are tumors which contain “cells from the ectodermal, mesodermal and endodermal layers”2,3 although this definition shifting toward “a mass composed of any two germ layers”1,4 or even monodermal.5 These neoplasms also are referred to by a multitude of other names, including dermoid cyst, dermoid cyst of ovary, dermoid ovarian cyst, benign cystic teratoma, mature teratoma, mature cystic ovarian teratoma, and ovarian mature cystic teratoma. The most common age for occurrence of teratoma is younger women, primarily between 30-40 years of age, although they may occur at any time of life.6 Ovarian teratomas are common, and make up 20% of adult ovarian tumors.7 There are many theories of pathogenesis, including misdirection or entrapment during migration.4,5 Germ cell tumors are most commonly located in the gonadal area [ovaries, testicles5] but are rarely found in extragonadal tissue, mediastinum,3,5,8,9 presacral,10 sacrococcygeal (immature type in infants),11,12 pineal gland,9 retroperitoneum,8,9 neurohypophysis,1 kidneys,11 spinal,12,13 urachal.14 Teratomas are frequently asymptomatic and often diagnosed as an incidental finding when imaging is obtained for other reasons.15–17 Kaeser et. al. describes the differential diagnosis of calcific abdominal masses.1
CASE REPORT
A 25-year-old woman was being treated in a chiropractic outpatient clinic for low back pain. The teratoma was an incidental finding on radiography as she did not improve with standard care. Table 1 summarizes her clinical findings and symptoms (CC,OPPQRSTA) and past, family, social history (PFSH) pattern. Ovarian teratoma subjective information was not compared since they are normally asymptomatic.1,15–17
As noted, an incidental finding of a pelvic calcific density was discovered on radiography (Fig 1) which led to the working diagnosis of teratoma.
Management and Outcome
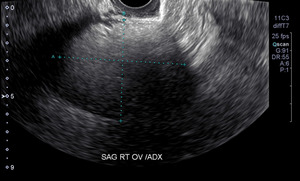
We referred our patient to a gynecologist at the recommendation of the chiropractic radiologist that read the films. To confirm the suspected diagnosis, the gynecologist referred the patient for ultrasound imaging (Fig 2). The patient then underwent an oophorectomy. Although the risk is relatively small (0.8%-5.5% of cases), there does exist a chance for malignant degeneration.1,15–17 She reports infrequent, mild low back pain post-surgery.
Discussion
Several considerations arise from this case relative to patient management within a chiropractic outpatient setting. Radiographic image was initiated with the involvement of the patient, which serves as a reminder that the patient is an integral part of the diagnostic process. Additionally, Youngs terminology of an “incidentaloma” is applicable here.18 Field clinicians who are both receiving and making referrals to other healthcare practitioners should be aware of the differing terminology used across all healthcare disciplines.
In addition, this case echoes the importance of understanding the need for referral and co-management to ensure proper patient care. Outlined by Globe, et. al, this patient was referred as soon as a tumor was discovered since it fell into the Globe et als’ category of “Conditions Contraindicating Certain Chiropractic-Directed Treatments Such as Spinal Manipulation and Passive Therapy”.19 In this case, a calcific density suggesting teratoma with slight chance of malignant degeneration resulted in referral that ultimately led to a preventative surgery. As noted by both Sahin and Gaducci, it is possible that teratomas will undergo malignant degeneration.15,17 For practitioners that may encounter these in clinical practice, note that “having first-degree relative with mature cystic ovarian teratoma may be associated with increased risk for mature cystic teratoma”.6 For patients that undergo surgical excision of teratomas, it is also possible that they may redevelop. This recurrence appears to be dependent on a multitude of factors that have been investigated in several papers. Age may be a factor in the recurrence rate. Tokamak et al, found that mature cystic ovarian teratomas recurred in 4.5% of women who underwent surgery, while Rogers, et al., found a recurrence rate of 10.6% in pediatric and adolescent patients that underwent cystectomy procedures.20,21
Our patient improved and valued chiropractic care though the cause of the improvement was unknown due to the questionable temporality of the association. As this is an isolated case study, the information included in this case should not be over generalized and instead viewed as an opportunity to discuss the importance of identification and proper co-management of incidental findings within an outpatient setting.
The “take home” lessons are1 Chiropractors may consider radiography of patients when not improving. Some findings such as calcific densities in females may be incidental yet important.2 With calcific densities in the abdominal cavity in a female, consider teratoma and refer to a gynecologist due to slight risk of malignant degeneration. And3 After recovery from surgery, the patient reported improvement of her chronic, non-responsive low back pain; causality unknown.
Consent
Written consent for this publication was obtained from the patient. IRB Assurance #N2018-2-20-M with exemption.
Competing Interests
The authors declare no competing interests.